Certain ICD-10 codes are used not to describe a single disease, but to capture patterns of metabolic abnormalities that frequently occur together. At HealthSure Hub, we focus on providing clear, code-specific information that helps explain how these classifications are used within medical records and healthcare data systems.
One such classification is ICD-10 code E88.81, which is assigned to metabolic syndrome and other forms of insulin resistance. Stay as we break down the code and elaborate more on why proper documentation is crucial when it comes to this code in particular.
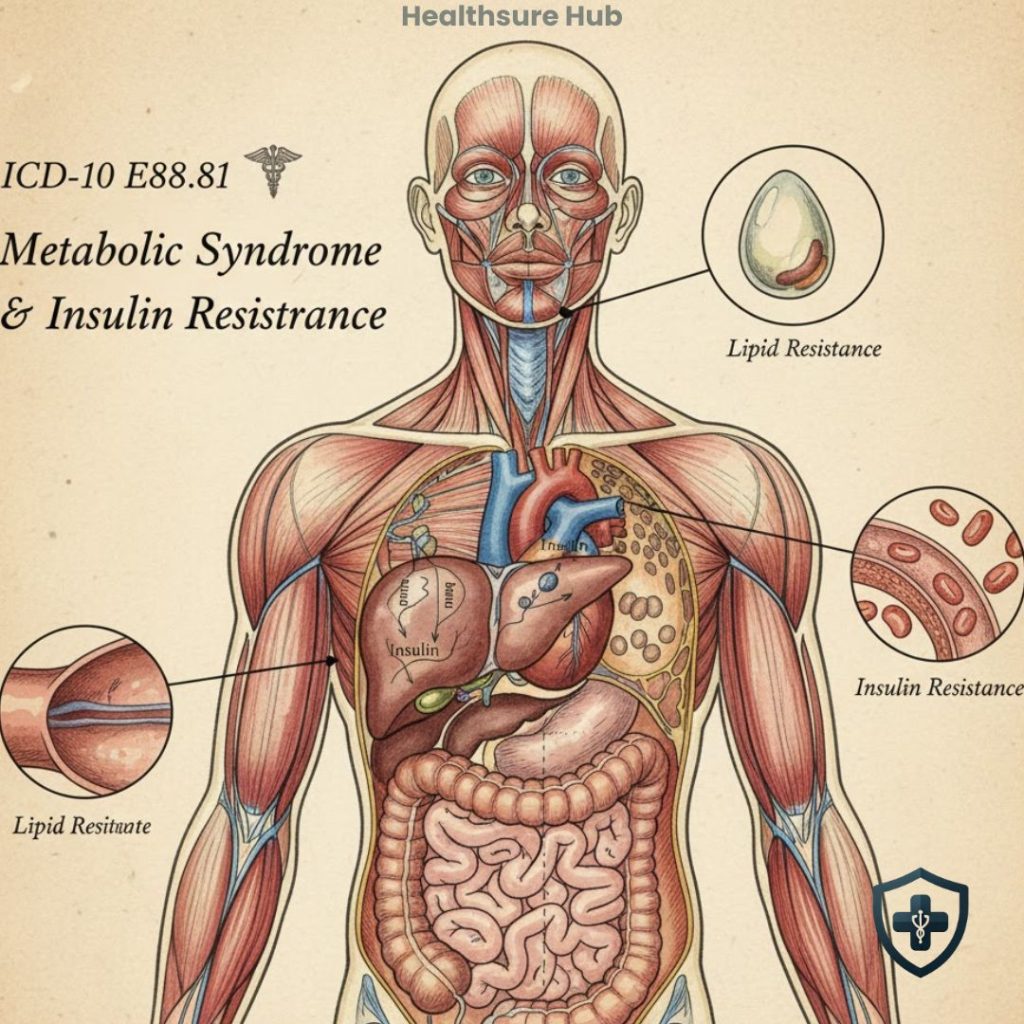
Overview of ICD-10 Code E88.81
E88.81 is categorized as another specified metabolic disorder. This code falls under the Endocrine, Nutritional, and Metabolic Diseases chapter (E00–E89), specifically in the block for Other disorders of metabolism (E88).
Its primary function is to identify patients who present with metabolic syndrome or insulin resistance without the presence of another primary endocrine disorder, such as type 2 diabetes mellitus. Unlike codes for diabetes or hyperlipidemia alone, E88.81 is designed to capture the combination of metabolic abnormalities that constitute metabolic syndrome.
As a billable ICD-10 code, E88.81 allows healthcare providers to document these conditions in patient charts, which supports medical record accuracy and healthcare analytics. While clinical evaluation determines the presence of metabolic syndrome, E88.81 provides a standardized way to record this diagnosis for administrative purposes.
Structure of ICD-10 Code E88.81
| Code Element | Meaning |
| E | Indicates diseases of the endocrine, nutritional, and metabolic systems |
| E88 | Represents other disorders of metabolism |
| .8 | Identifies other specified metabolic disorders |
| 1 | Specifies metabolic syndrome and other insulin resistance |
Clinical Context for E88.81
The use of E88.81 is appropriate when a patient exhibits documented clinical features of metabolic syndrome or insulin resistance that are not secondary to another primary condition. Common features associated with this code include:
- Central obesity: Typically measured through waist circumference.
- Elevated fasting glucose or insulin levels: Indicating reduced insulin sensitivity.
- Dyslipidemia: Characterized by high triglycerides and low HDL cholesterol levels.
- High blood pressure: Often present in combination with other metabolic syndrome features.
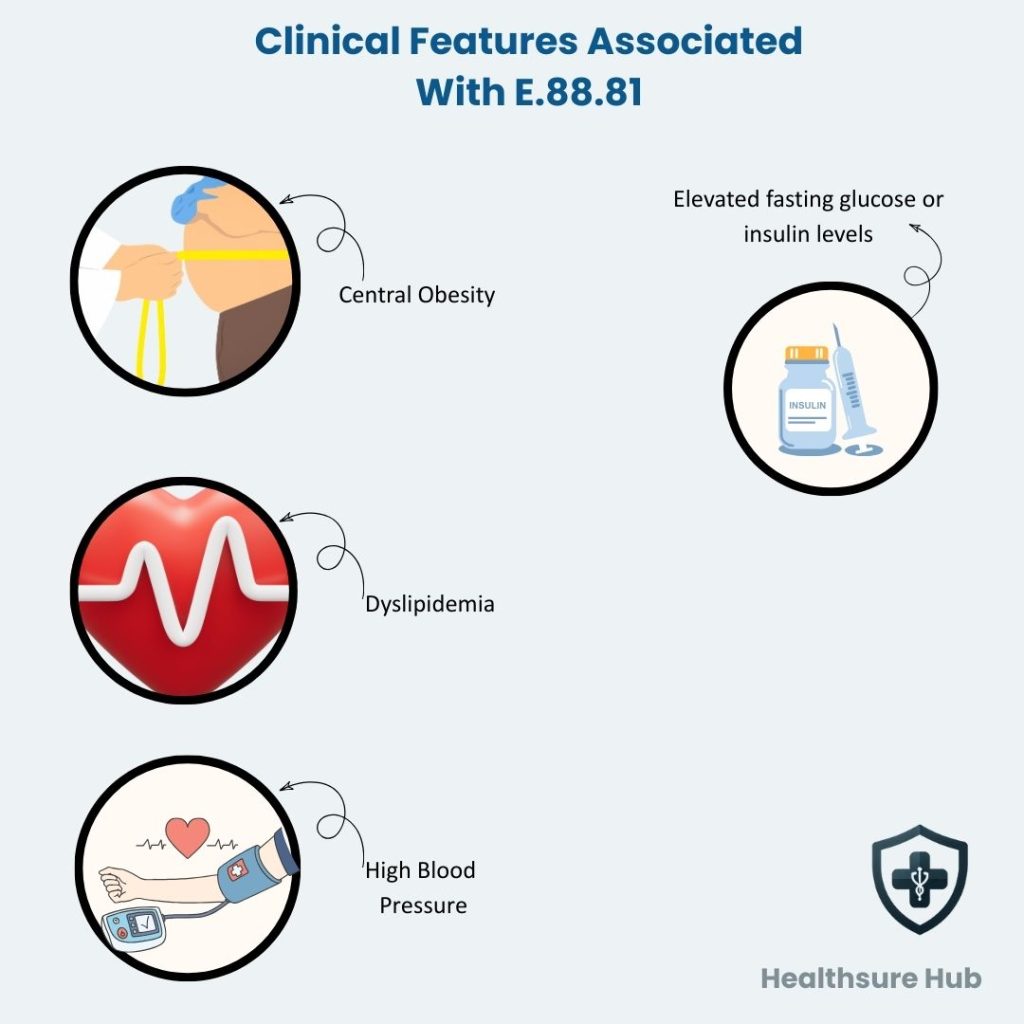
This code can be applied as either a primary or secondary diagnosis depending on the context of the patient visit. For example, a patient may be treated primarily for hypertension but have documented insulin resistance; in this case, E88.81 would appear as a secondary code. Accurate coding requires that each feature of metabolic syndrome or insulin resistance is clearly documented in the medical record.
Real-World Statistics on Insulin Resistance
Understanding the prevalence of insulin resistance can highlight why accurate documentation is critical:
- Roughly 26.5% of the global adult population exhibits some degree of insulin resistance, with estimates ranging between 26% and 30% across regions.
- Certain populations—including Mexican Americans, South Asians, and Aboriginal groups—show higher susceptibility.
- In the U.S., studies suggest about 40% of adults are insulin-resistant, with one analysis reporting that 40% of adults aged 18–44 exhibit signs of insulin resistance.
- Insulin resistance significantly increases the risk for type 2 diabetes, cardiovascular disease, and non-alcoholic fatty liver disease.
Documentation Notes
Proper documentation is essential for accurately applying E88.81. This includes:
- Anthropometric measurements: Body mass index (BMI) and waist circumference.
- Laboratory results: Fasting glucose, insulin, triglycerides, and HDL cholesterol levels.
- Clinical notes: Explicit mention of insulin resistance or metabolic syndrome features.
Documentation ensures the code reflects the actual metabolic abnormalities present in the patient, which is crucial for maintaining accurate medical records and supporting data consistency.
Risk Factors and Contributing Conditions
Metabolic syndrome and insulin resistance, captured under ICD-10 code E88.81, arise from a combination of genetic, lifestyle, and environmental factors. Understanding these contributors helps clinicians identify at-risk patients and implement preventive strategies.
- Genetics – family history plays a significant role. Individuals with parents or siblings who have type 2 diabetes, obesity, or metabolic syndrome are more likely to develop insulin resistance. Certain gene variants can influence how the body processes glucose and stores fat.
- Lifestyle – sedentary behavior, poor diet high in refined sugars and trans fats, and insufficient physical activity significantly increase the risk. Excess caloric intake and low activity contribute to central obesity, which is a hallmark of metabolic syndrome.
- Ethnicity certain populations, including Mexican Americans, South Asians, and Aboriginal communities, show higher susceptibility to insulin resistance due to genetic predisposition and environmental factors.
Accurate use of ICD-10 code E88.81 is not just clinically important—it also has significant implications for insurance and billing. Proper coding ensures that healthcare providers can document care accurately and receive appropriate reimbursement.
Insurance and Billing Considerations
Accurate use of ICD-10 code E88.81 is not just clinically important, it also has significant implications for insurance and billing. Proper coding ensures that healthcare providers can document care accurately and receive appropriate reimbursement.
- Impact on Claims – E88.81 helps insurers understand the patient’s full clinical picture. For example, a patient treated for hypertension or hyperlipidemia who also has metabolic syndrome can have E88.81 listed as a secondary diagnosis. This ensures that claims reflect the complexity of the patient’s condition and the care provided.
- Compliance and Reimbursement – accurate documentation of metabolic syndrome and insulin resistance is essential for compliance with healthcare regulations and coding standards. Misreporting or omitting E88.81 could result in claim denials or reduced reimbursement.
- Supporting Preventive Care Coverage – Some insurance plans may provide coverage for lifestyle interventions, nutrition counseling, or preventive medications for patients with metabolic syndrome. Using E88.81 correctly can justify these services to insurers, making preventive care more accessible.
Example of Use
A typical scenario for E88.81 might include the following:
- Patient: 52-year-old male
- Measurements: BMI 32, waist circumference 105 cm
- Lab results: Fasting glucose 108 mg/dL, triglycerides 210 mg/dL, HDL 38 mg/dL
- Blood pressure: 135/88 mmHg
- Clinical documentation: “Metabolic syndrome with features including insulin resistance, dyslipidemia, and hypertension.”
In this case, the corresponding ICD-10 codes would be:
- Primary: E88.81
- Secondary: I10 (Hypertension), E78.5 (Hyperlipidemia)
This example demonstrates how E88.81 is used to record the presence of metabolic syndrome while allowing for other associated conditions to be coded appropriately.
Conclusion
ICD-10 code E88.81 serves as the official classification for metabolic syndrome and other insulin resistance disorders in medical records. It provides a standardized method for documenting these conditions, supporting administrative, reporting, and statistical functions within healthcare systems.
While clinical diagnosis identifies the syndrome, E88.81 ensures that it is systematically recorded, enabling accurate data collection and analysis. Its application across healthcare settings contributes to consistent medical record-keeping and research on metabolic disorders, making it a vital component of modern medical coding.


