ICD-10 code M25.559, which represents pain in the unspecified hip, is commonly used in medical billing when a patient reports hip pain but the clinical documentation does not specify whether the pain is on the right or left side. It is also used when no confirmed diagnosis has yet been established at the time of the encounter.
Although it is a valid diagnostic code, M25.559 is best understood as a temporary or transitional classification that reflects incomplete diagnostic detail rather than a definitive clinical condition.
Understanding What M25.559 Represents
From a coding perspective, the ICD-10 code falls under musculoskeletal symptom codes. M25.559 is a billable code for unspecified hip pain. These codes describe patient-reported symptoms rather than confirmed diseases. In this case, the provider has documented hip pain, but the record does not include laterality or an underlying confirmed cause such as arthritis or injury.
This type of code is most often seen in early-stage evaluations, especially when diagnostic testing has not yet been completed or reviewed. It allows claims to be submitted while clinical investigation is still ongoing.
When M25.559 Should Be Used
The correct use of M25.559 depends entirely on the quality and specificity of the clinical documentation. It should only be assigned when hip pain is clearly documented, but no further detail is available to assign a more specific code.
In many cases, this occurs during a patient’s first visit or initial workup. However, once additional information becomes available, such as imaging results or a more precise clinical assessment, coders are expected to update the diagnosis to reflect that specificity.
Why Specificity Matters in ICD-10 Coding
ICD-10 coding guidelines require that diagnoses be reported at the highest level of specificity supported by the medical record. For hip pain, this means that laterality should always be captured when documented.
If the provider specifies that the pain is in the right or left hip, the correct codes would be M25.551 or M25.552 instead of the said code for unspecified hip pain. Using an unspecified code when more precise information is available is considered a documentation mismatch and can lead to claim delays or payer inquiries.
The Role of Documentation in Coding Accuracy
Accurate use of M25.559 is entirely dependent on provider documentation. Coders are not permitted to assume missing details, even if they seem clinically obvious. The medical record must explicitly support the code selection.
Good documentation typically includes a clear description of the pain, any associated clinical findings such as reduced range of motion or tenderness, and the provider’s assessment and plan. When this level of detail is missing, unspecified codes like M25.559 may be used, but they should not become a routine default.
Symptom Coding Versus Confirmed Diagnoses
It is important to understand that M25.559 represents a symptom, not a confirmed diagnosis. As such, it should only be used while the clinical picture is still developing.
Once a definitive diagnosis is established, such as osteoarthritis, bursitis, or another musculoskeletal condition, the symptom code should be replaced. Continuing to use a symptom code after a diagnosis has been confirmed can lead to inaccuracies in claims processing and may affect compliance reviews.
Medical Necessity and Billing Considerations
In medical billing, ICD-10 codes must support the medical necessity of any services provided. This includes office visits, imaging studies, and any procedures related to the patient’s condition.
M25.559 can support these services when hip pain is the primary reason for the encounter. However, because it lacks specificity, payers may require additional documentation to justify more advanced services, particularly imaging or specialist referrals.
Use of M25.559 as a Primary Diagnosis
M25.559 may appropriately be used as the primary diagnosis when hip pain is the main reason for the visit and no more specific diagnosis is available at that time. This is common during initial evaluations.
However, repeated use of this code across multiple visits without diagnostic progression can raise questions during claim review. Payers may expect to see the diagnosis evolve as additional clinical information becomes available.
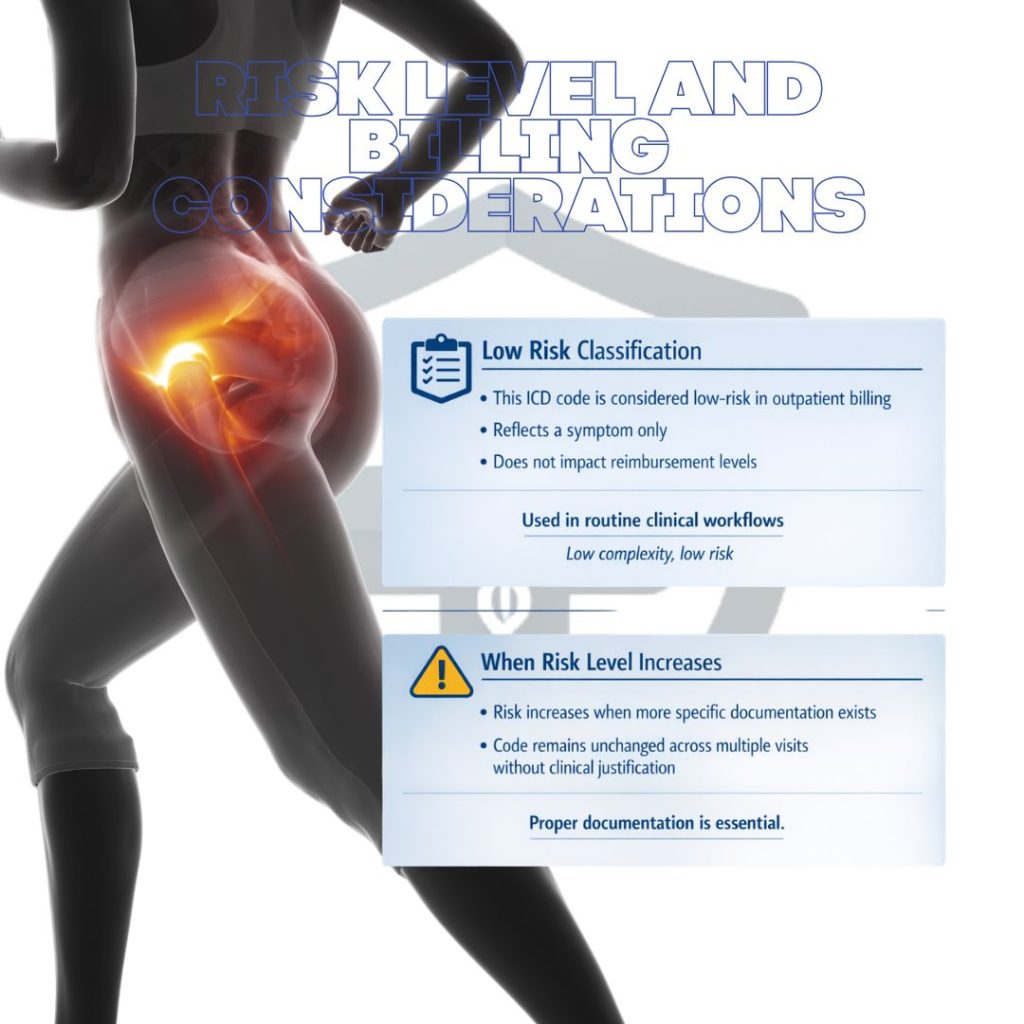
Risk Level and Billing Considerations
In most outpatient billing environments, this code is considered a low-risk code because it does not directly impact reimbursement levels and is commonly used in routine clinical workflows. It simply reflects a symptom rather than a high-complexity or high-cost diagnosis.
That said, the risk level can increase if the code is consistently used when more specific documentation exists in the medical record or if it remains unchanged over multiple encounters without clinical justification.
Prior Authorization Scenarios
Prior authorization may be required when this specific ICD-10 code is used to justify more advanced services such as MRI scans, CT imaging, or orthopedic referrals, depending on payer policies.
Because the code does not provide detail on severity, laterality, or underlying cause, insurers often request additional documentation before approving higher-cost services.
Common Billing and Coding Issues
Errors involving this code usually occur due to incomplete documentation or failure to update diagnoses as clinical information evolves. One of the most common issues is continuing to use unspecified coding even when laterality is clearly documented in the medical record.
Another frequent issue is failing to align diagnosis codes with the procedures being billed, which can result in claim delays even claim denials or requests for additional information.
Best Practices for Accurate Use
Accurate coding begins with complete and precise clinical documentation. Providers should ensure that laterality and relevant clinical findings are always recorded. Coders, in turn, should regularly review records for opportunities to improve specificity and update codes when new information becomes available.
Using structured documentation approaches and periodic coding audits can significantly improve claim accuracy and reduce unnecessary use of unspecified codes.
Conclusion
ICD-10 code M25.559 plays an important role in early-stage evaluation of hip pain, but it should always be treated as a temporary classification. Its proper use depends on accurate documentation, correct application of ICD-10 specificity rules, and timely updates as the clinical picture becomes clearer.
When used appropriately, it supports smooth claim submission during initial evaluation. When overused or left unupdated, it can signal gaps in documentation quality and affect billing efficiency.


